Dermatology
Psoriasis - There are ways to prevent and minimise discomfort
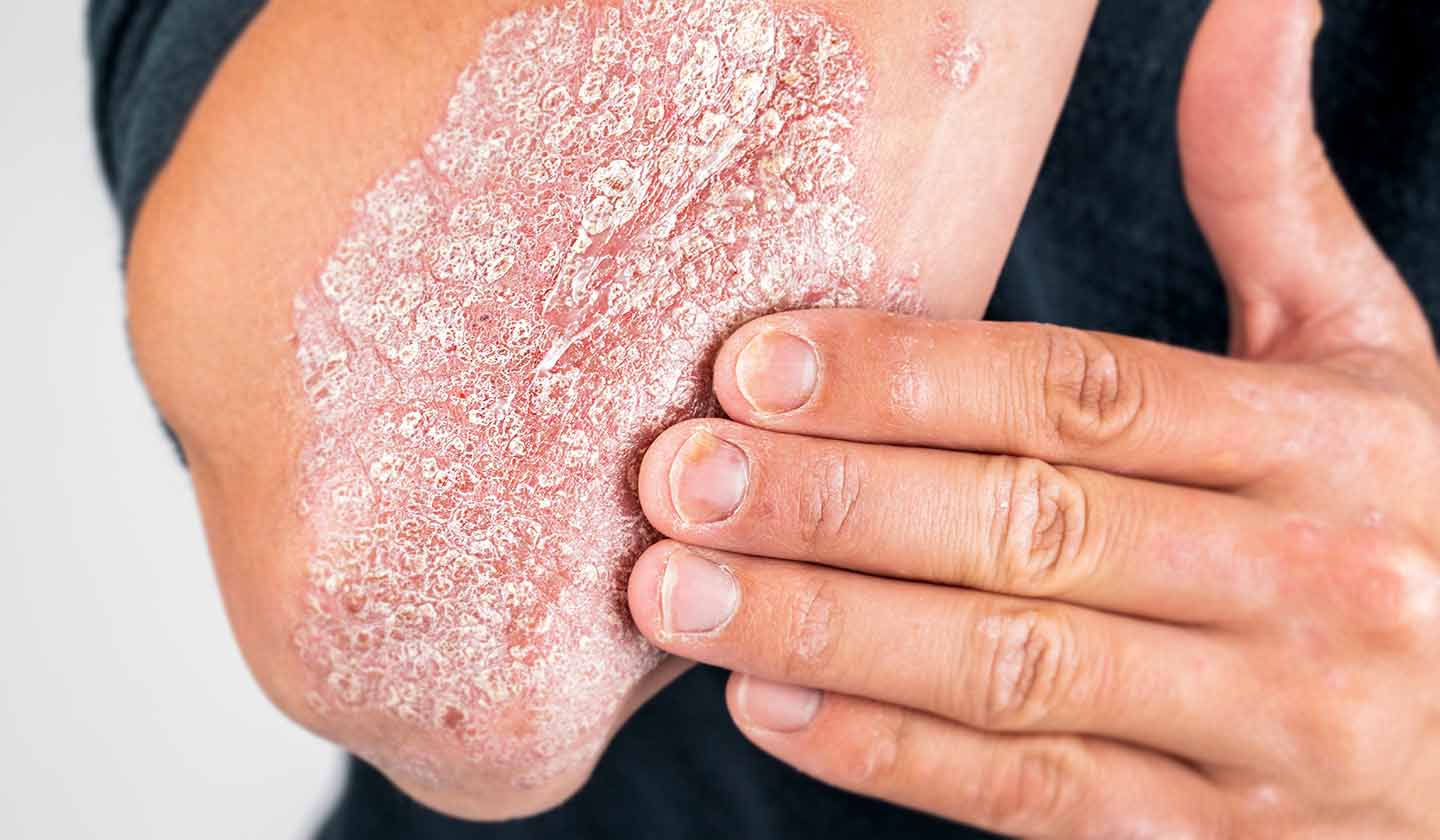
Psoriasis is a benign, chronic inflammatory skin disease, related to genetic transmission, that needs triggering factors to develop in the body. It affects 1 to 2% of the world population. There are two age peaks of prevalence: before the age of 30 and after 50, and in 15% of cases, it appears before the age of ten.
How does it develop?
It is a non-contagious, multigenic disease (it needs several genes for its development), and partly dependent on external factors. The disease can present different clinical forms and different degrees. The onset of the disease can occur at any age, being triggered by the environment, the use of some medications or stress. In people with a family history, the onset seems to occur earlier.
What does it feel like?
The injuries are very typical, with periods of exacerbation and remission, located mainly on extension surfaces, such as knees and elbows, scalp, palms, soles of the feet (areas of major trauma).
Psoriasis types are named according to their location and appearance, and can be divided into:
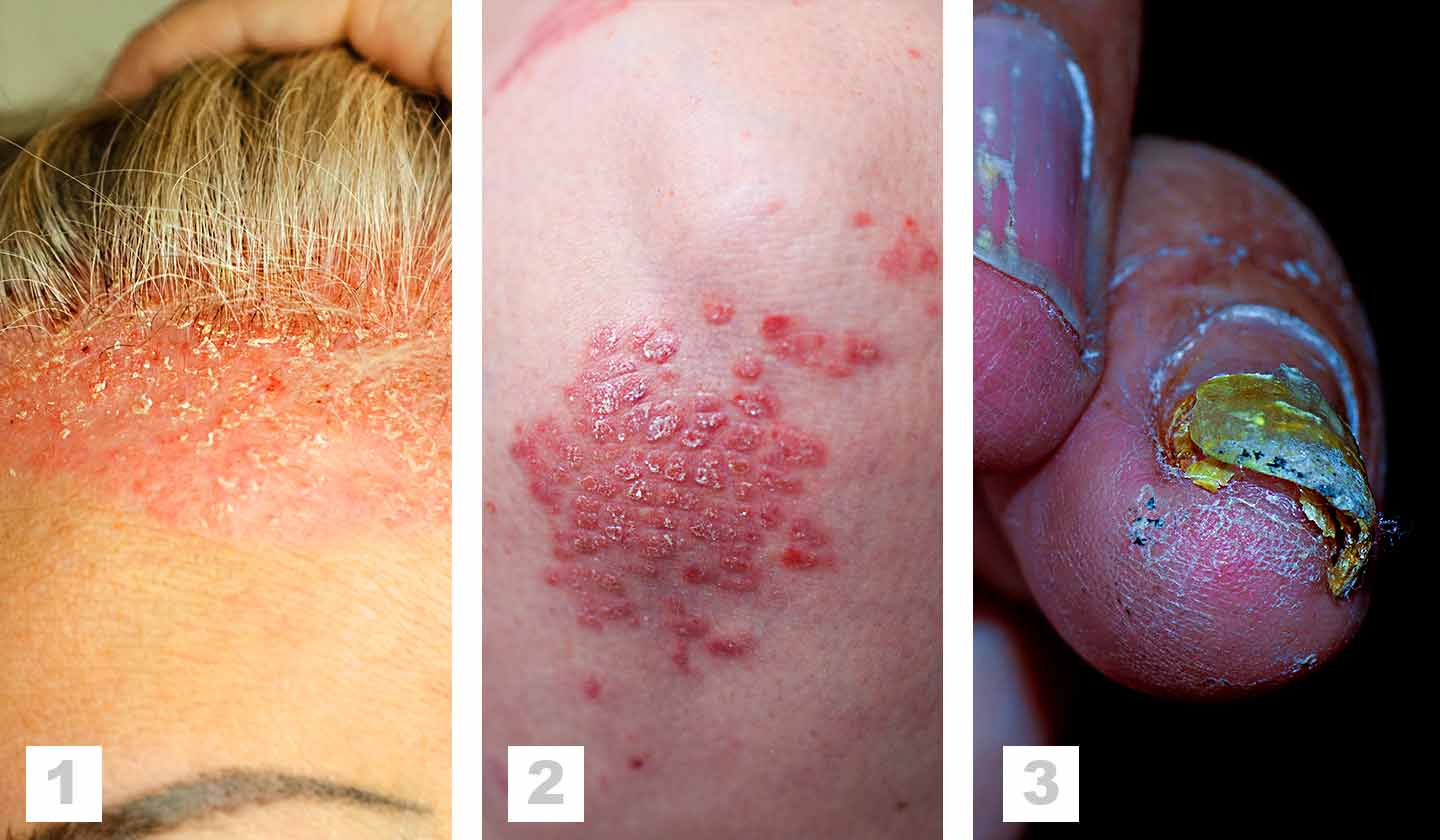
- Psoriasis vulgaris - It presents varying sized, well defined, reddish patches with dry adherent scales, which can be silver or grey, and the most commonly affected areas are the scalp, elbows, and knees.
- Guttate psoriasis - Teardrop-shaped spots associated with infectious processes. The lesions are small, located on the trunk and proximal part of the arms and thighs (closer to the shoulders and waist), sparing hands and feet. This type of psoriasis is characterized by numerous lesions that appear abruptly, with a higher prevalence among children and young adults.
- Nail psoriasis - It can occur as an isolated episode, affecting the nails of the hands more often than the toes. Characteristic but not specific features of this condition include punctate depressions or yellowish oil-coloured spots; there are also other less common nail changes.
How is it diagnosed?
The diagnosis is generally easy, being based on the patient’s clinical history, observation of typical lesions with characteristic data obtained from skin scraping and medical examination.
In more severe cases or unusual forms, a skin biopsy (skin exam with a characteristic or indicative diagnosis) can be performed.
Some laboratory tests can help the investigation of triggers of the disease (such as diabetes and a bacterial infection caused by streptococcus).
How to treat it?
It is important to provide general guidance regarding the disease, individualising treatment according to the characteristics of each patient. The patient should be reminded of the non-contagious aspect of the disease, the triggering factors, such as stress, cold, excessive exposure to the sun, some diseases (uncontrolled diabetes, infectious outbreaks), and the use of some medications.
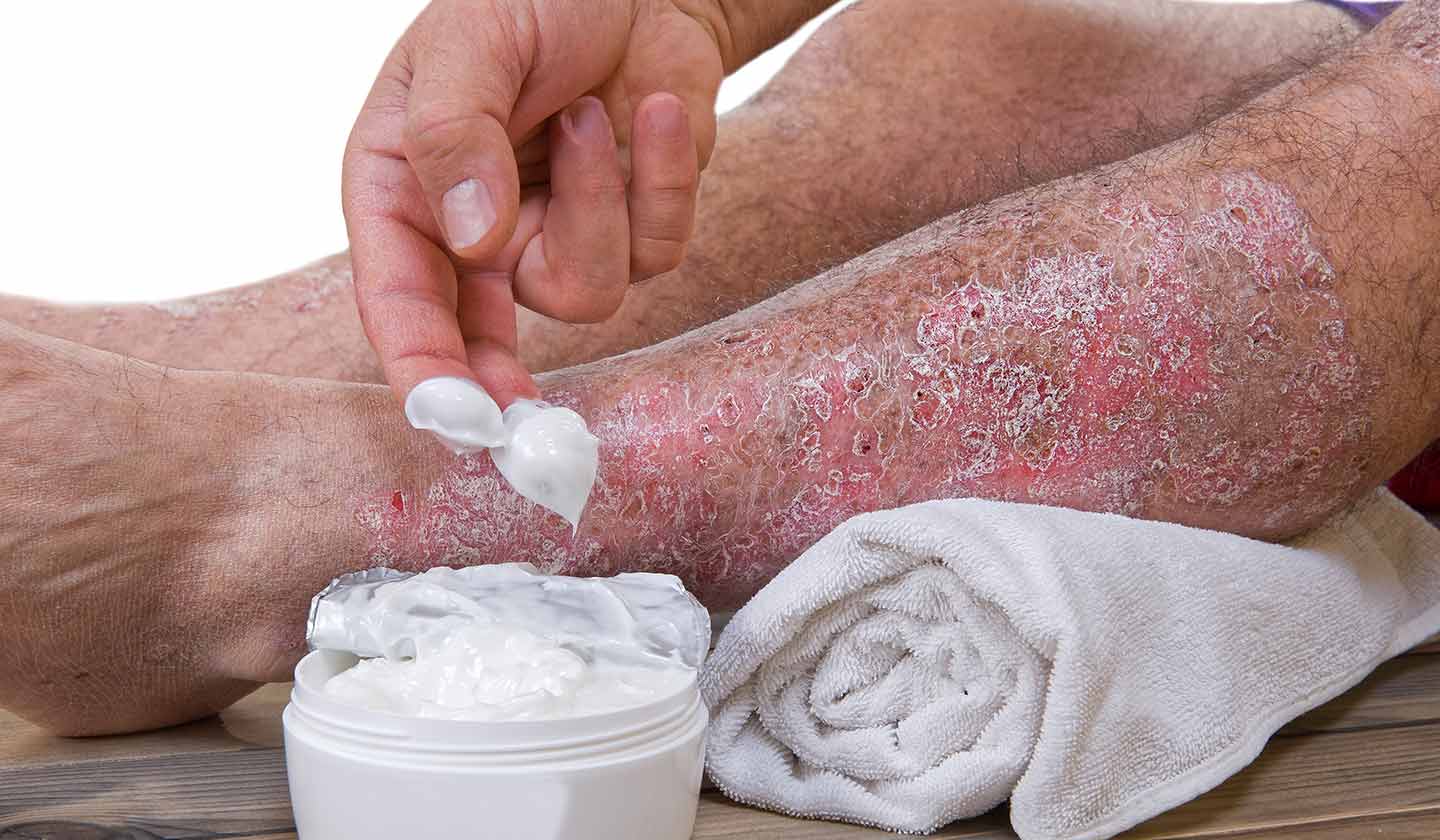
Mild to moderate cases (75% to 80% of cases) can be controlled with medication for local use, applied onto the skin, which should always be prescribed and controlled by the doctor.
Moderate sun exposure and continuous skin hydration are essential to most patients.

António Hipólito de Aguiar
(Pharmacist; University Professor)
Também lhe poderá interessar
Endocrine system
Diabetes - When your body doesn't know what to do with sugar
Neurology






